Ask a professional: insights from an OT
Name: Cassie Doyle
Role: Senior Occupational Therapist
Cassie is one of the Senior Occupational Therapists at CPEC. Describing herself as “crafty”, Cassie graduated from LaTrobe University with a Bachelor of Occupational Therapy (2011) and a Master of Advanced Occupational Therapy (2016). Cassie started her OT journey by working with children and young people in education, then community health, before landing at CPEC in 2018. Cassie is trained in home modifications, transportation of children with disabilities in motor vehicles, BoHA assessment, SOS approach to feeding and Learn to Play.
Cassie is passionate about physical disability and neuromotor disorders and creating a community of people around the child that can see the potential and possibilities for the future. Cassie thrives when engaging families for the first time and starting the therapy journey alongside them. When she isn’t at CPEC, Cassie loves paddle-boarding, reading and playing netball.

The most rewarding thing about my work is the moment where a child sees themselves as someone who can do things, whatever that looks like for them, and their parents get to see their child’s joy and excitement in being an active person
Q&A
- Can you share some insights into your role and work with disabled children? What drew you to this field, and what is most rewarding about your work?
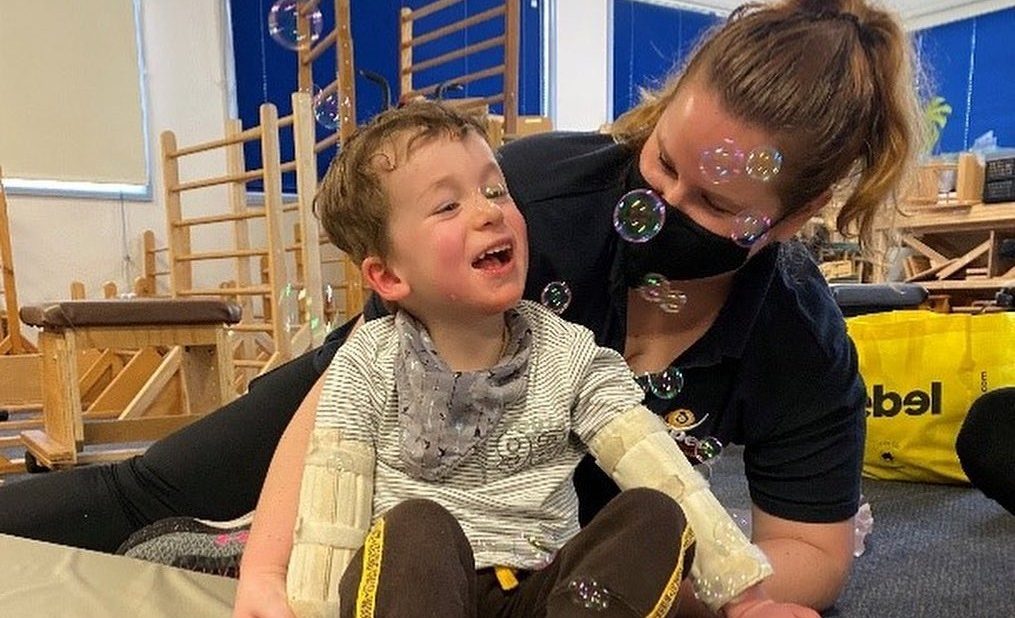
I’m an occupational therapist working with children and young people with cerebral palsy and other physical disabilities. I see my role as supporting children and families to do all the things they want and need to do. My mum was an integration aide, and that drew me to working with kids with physical disabilities. The most rewarding thing about my work is the moment where a child sees themselves as someone who can do things, whatever that looks like for them, and their parents get to see their child’s joy and excitement in being an active person. Like when I was supporting a 4yo boy with very little active movement, his parents didn’t think he could really do anything. We set up a switch with some music, and he could do the tiniest little movement of his hand to play the music. And then he did it again and again, and the joy on his mum’s face as she saw her son playing was something that I will never forget.
- What common challenges do professionals in your field face when working with disabled children? How do you address these challenges and ensure the best care and support for the children and their families?
Challenges can come from all directions: funding delays, difficulty accessing equipment, and supporting families who are experiencing grief and maybe aren’t ready for change.
As a clinician, I come in with open expectations of children and their families, and I’ll meet them where they are. Having clear goals developed with the family ensures we’re all working in the same direction. It also means I can support families in navigating the more complex systems around disability, like NDIS, which can be very frustrating and overwhelming. Communication and open expectations are the keys to supporting families effectively.
One of the significant challenges in the industry at the moment is everyone working in silos – so many private practices, so little time to talk and collaborate, and parents pulled in all different directions. Working in a transdisciplinary team helps me clarify my role as an OT. It embeds the approach from the child’s speech pathologist and physiotherapist into my practice, so we can reinforce the same strategies to help the child and the family learn. I want to ensure that I collaborate with everyone working with the child – family, kinder, school, and other therapists – so we’re all on the same page. I can imagine it’s so difficult for parents to have therapists giving contrary advice to each other, and working in a team means we can help prevent that.
- In your experience, what are some effective strategies or interventions that have helped improve the quality of life for disabled children? Are there any specific approaches or techniques you find particularly beneficial?
I see the most effective changes when children and families embed therapy strategies into everyday life. We have to make the movement meaningful. Sure, a child can do five sit-to-stands, but if they do an active transfer every time they get out of their wheelchair, they get the same practice with the added bonus of feeling active, empowered and in control. Good quality, 24-hour positioning is important, as is understanding and meeting sensory needs. I said earlier that communication is key – that’s true for families and also for children with disabilities. Augmentative and Alternative Communication is a vital part of therapeutic input for those unable to use speech to meet their communication needs.
- How do you collaborate and communicate with parents or caregivers of disabled children? How do you involve them in decision-making and ensure their voices are heard?
When I first meet a family, I always tell them, “If anything I’m saying doesn’t make sense, tell me. Tell me if I say something and you know that you’re not going to do it, or it doesn’t fit for you. I don’t want you to feel like you’re wasting your time or like you have to pretend at clinic then go home and do nothing.”
I like to have this chat with them right from the start, so there’s always a back-and-forth, open communication.
We set goals regularly and check in about them. At the start of most sessions, I’ll ask the family if there is anything they want to work on, and at the end, I’ll ask if we missed anything. If I’m not seeing the skill progression I’d expect, I’ll ask the family how practice at home is going, and we can problem-solve it together. If I see more skill progression than expected, you better believe we’re celebrating!
Also: listen. Listen to what families are saying and listen to what they aren’t saying. When families start not showing up to sessions, or not wanting to talk about things, or having difficulty using equipment, that’s telling you something. My job is to create a space where they feel comfortable talking about it and help find a way to move forwards together.
The other super important part is working with the child to communicate their goals, ideas and thoughts. When a child chooses something or communicates something, it’s so powerful and can help both therapists and parents remember what it’s all about and where we’re headed.
- What improvements would you like to see in your profession or industry to improve your ability to care for and support disabled children and their families?
I would love to see a more streamlined team approach in early intervention. Parents are so overwhelmed by information and choice, often at a stage in their journey where they are grieving and just learning about their child’s disability. I’d like to see more support and guidance for parents in the early intervention space. As an OT, it would also be great to spend a lot less time reporting and submitting funding requests and have a lot more time to do actual capacity-building therapy.
You can follow Cassie and her colleagues’ work @
Facebook – https://www.facebook.com/CerebralPalsyEducationCentre
Instagram – https://www.instagram.com/cpec.therapy/






